Vomit, spiting and sexual assaults - what our A&E staff face as alcohol fuels injuries and disorder


That is the message from medics and experts who are dealing with their busiest run of shifts during the festive period.
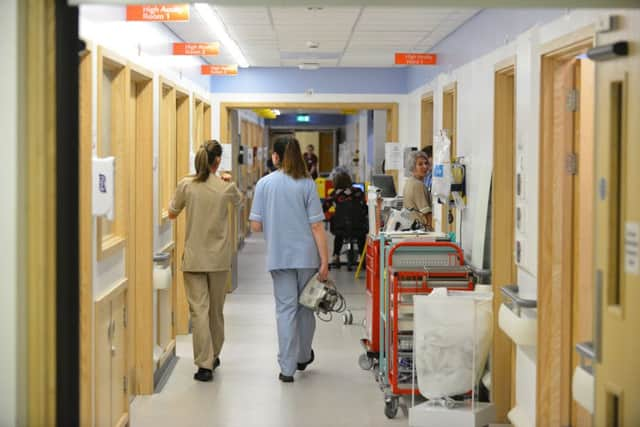
Staff at Sunderland Royal Hospital have told of patients so drunk they have urinated in sinks, lay on the floor in their own vomit or exposed themselves to workers after suffering harm because of their own drinking.


Advertisement
Hide AdAdvertisement
Hide AdHead injuries and damage caused by assaults and falls are among the most frequent reason why people end up in the emergency department, before then causing trouble for staff and disrupting the care and treatment of other patients.
While many are aged 18 to 30, Sunderland Royal Hospital has seen a rise in the number of 40 to 50-year-olds seeking help because of drink-related issues, with women wine drinkers, who add to their regular consumption when out for the night.
Doctors and staff at Balance, the North East Alcohol Office, are calling on the Government to rethink how it deals with the producers of alcohol and enforce a minimum 50p a unit price for drink.
It comes after the Echo recently reported that, in the region’s larger emergency departments, it is common for staff to treat 30 to 40 patients a day who have been drinking, diverting resources from other cases and placing a huge strain on resources and the staff themselves.

Advertisement
Hide AdAdvertisement
Hide AdAt times, security guards are drafted in to help ensure safety for the workers and other patients, while the financial cost to hospitals across the region is estimated to run into millions.
Dr Kate Lambert, who has been based at Sunderland’s accident unit since 2002, is among those who worked on ‘Black Eye Friday’ and is preparing to work on some of the busiest shifts including New Year’s Eve.
She said: “We’ve had people who have been spat at, touched inappropriately, patients vomiting on them, on themselves, people urinating in sinks, lying on the floor in vomit.
“It’s behaviour you don’t expected in a hospital.


“When you’ve got a 93-year-old who’s got pneumonia and other people you should be helping and someone else is saying they’re going to leave when they haven’t been assessed and people have something seriously wrong with them, then it’s very difficult.
Advertisement
Hide AdAdvertisement
Hide Ad“Sometimes, when you speak to these people the next morning, and when they hear about their inappropriate behaviour, they can be quite taken aback.”
She said the team found the busy times and the abuse make the job hard, but that they all pull together and know that while patients may not say it when they are in a state of intoxication and distress, they know their part in the NHS is appreciated.
The team also ensures those in need of support to reduce their alcohol intake are given help.


Sue Taylor, partnerships manager with Balance, agreed something must be done to reduce the easy access to drink, especially alcohol such as cider.
Advertisement
Hide AdAdvertisement
Hide AdShe said: “What we are finding in Sunderland is that there is no down time for emergency departments, they are seeing presentations of people 24/7, not just peak times, in part to alcohol.
“A huge factor in that is down to drinking hours as well as people drinking at home.
“It cannot go on. There is no silver bullet.
“We want to see a minimum 50p a unit price. There’s a misconception that it will affect moderate drinkers, which isn’t the case, it will be people who are drinking cheap cider and those who tend to be dependent.
“Alcohol costs the North East £1bn and costs the NHS quarter of a billion a year and, in times of austerity, that’s a cost we cannot sustain,”